Science and technology day! That always makes me happy.
It’s amazing how much we’ve learned about the immune system response to Covid-19 in the six months since the disease first surfaced. Robert Plenge, an SVP at Bristol-Myers-Squib, put together an excellent Twitter thread that details the Covid-19 immune response story and suggests T-cell therapies that may be effective in extremely bad cases.
To help you through Plenge’s thread, here’s a quick, very high level ‘splainer on the B-cells and T-cells that make up our immune systems. B-cells create antibody proteins that latch on to a virus, usually slowing or disabling it. There are also B-memory cells that remember how to make antibodies.
T-cells play two roles. T-helper cells recognize antigens and signal an immune system response, including telling the B-cells to get to work. T-killer cells destroy infected human cells to stop viral replication.
Most of this science got worked out by researchers figuring out how HIV works. Here’s a pretty picture that explains the immune system response to Covid-19. It includes other components of the immune system like signaling proteins not described in the quick ‘splainer.
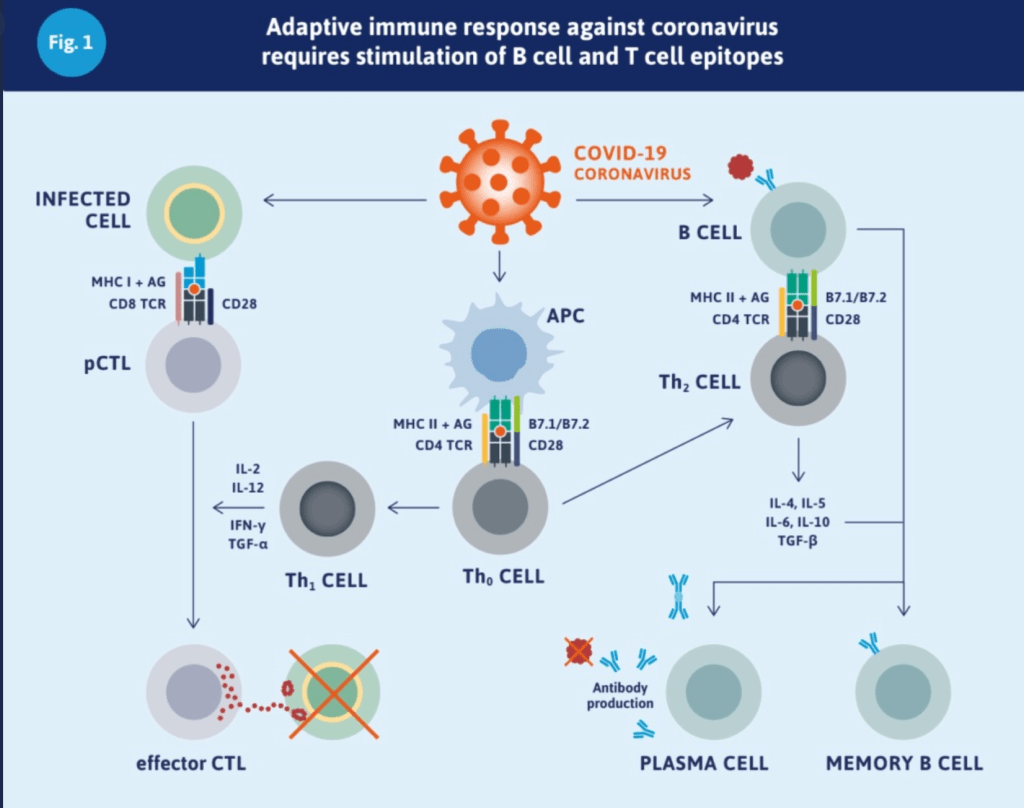
Plenge identifies two immune system conditions that may prevent immune systems from clearing Covid-19, and three other conditions that may provoke the immune system to go into overdrive.
Taken together, these five observations suggest that in COVID-19 patients with evidence of a maladaptive immune response, T cell-directed therapies may be beneficial in preventing progression to more severe disease.
Robert Plenge, SVP, Bristol-Meyers-Squib
If T-cell therapies can be developed for these five conditions, then Covid-19 mortality drops, mitigating the Covid-19 public health issue.
Now that you have a PhD in immune system response to Covid-19, here’s some good news. In spite of reports that some people may not develop Covid-19 immunity, it appears T-cells do, in fact, maintain Covid-19 immunity. In two small studies, researchers found T-cells that recognized the spike protein—the protein that enables Covid-19 to enter a host cell and replicate—in patients who’d recovered from mild cases of Covid-19. Not only that, but researchers also found that about a third of people who have not been exposed to Covid-19 have T-cells that recognize the SARS-Cov-2 virus, probably as a result of past exposure to other Coronaviruses.
If you were paying attention above, you noticed that B-cells produces antibody proteins that attack invading viruses. One of the biotech’s handy-dandy tools, monoclonal antibody (mAb) technology, takes advantage of the work B-cells have done by cloning antibodies already produced by an immune system. Here’s a whole article on Covid-19 mAbs.
There are two types of antibodies. Some antibodies bind to a virus, but leave it operational. Others bind in a way that gums up the viral works. They are called neutralizing antibodies and they are preferred candidates for mAb development.
There are at least five major efforts from Regeneron, AbCellera/Lilly, Vir/GSK, AstraZeneca, and Amgen/Adaptive to create cocktails of Covid-19 antibodies using mAb technology. Some cocktails will be in human trials next month, others are planning to ramp up production in the fall.
Sorrento announced last week that it found a human antibody that provides “100% inhibition of SARS-CoV-2 virus infection of healthy cells after four days incubation.” This is in the lab, mind you. The company plans to include the STI-1499 antibody, which neutralizes the Covid-19 spike protein, in its mAb cocktail.
Like the T-cell therapies Plenge discusses in his Twitter feed above, mAb therapies can be used to reduce Covid-19 mortality, mitigating Covid-19 public health issues. Whether mAbs can substitute for vaccines in the short term by providing Covid-19 prophylaxis is a provocative prospect.
Trump is telling the US that Covid-19 testing isn’t important. He’s saying that, of course, because he’s a salesman trying to draw attention from his dire shortage of Covid-19 tests.
Testing is crucial! Tests can help us diagnose Covid-19 infections, measure the effectiveness of vaccination, and assess immunity in a population
Here’s an article that gives the status of state-of-the-art of Covid-19 serological (antibody) testing. If you think vaccine development is hard, check out all the trade-offs involved in designing a Covid-19 test. To start with, there is test complexity, safety, sensitivity, and time to result. Then there are the fine points like whether to detect Covid-19 spike proteins or the viral nucleoproteins.
Scientists are figuring out which test method will best serve each testing application. Lots of them.
Several academic laboratories have developed robust, specific serological assays, and high-quality commercial options are becoming available. In accordance with academic grassroots traditions, a toolkit to set up antibody assays has been distributed to more than 200 laboratories across the world, and a detailed protocol to facilitate local implementation has been published
Science, “Measurement of antibodies to SARS-CoV-2 will improve disease management if used correctly,” 15 May 2020.
The bad news is that current antibody testing is a mixed-bag. The good news is that 200 laboratories around the world are working on better Covid-19 tests.
Should we worry about Covid-19 mutations? The Nextstrain Situation Report provides a genomic analysis of Covid-19.
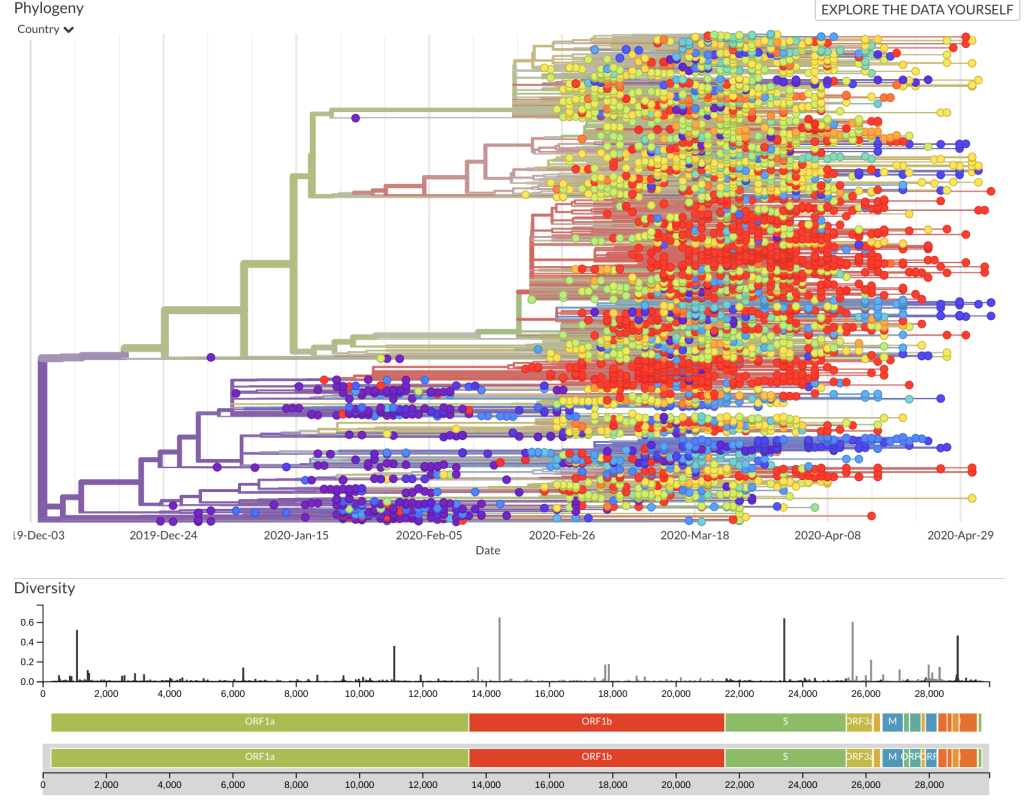
We’re in good luck here because the rate and type of Covid-19 mutations are in line with other Coronaviruses.
The report describes Covid-19 international transmission in terms of “sparks.” Sparks fly from an outbreak to other locations where most of the sparks fizzle out, but some start a new outbreak that then creates more sparks.
Unsurprisingly, we see this pattern in countries experiencing their first wave of infections. More alarmingly, we also see this pattern after re-introductions of the virus to countries where the initial peak passed months beforehand. Ultimately, this pattern is only broken when a country is able to effectively test, trace, and isolate cases immediately.
Nextstrain Situation Report, 15 May 2020
In other words, we can’t eradicate Covid-19 on a country-by-country basis. We have to do it worldwide.
Science is great, but how do we get it from the lab to clinicians around the world? That’s a whole different problem.
Let’s say there’s a drug that speeds recovery from Covid-19. How effective is that drug if doctors don’t have adequate information to know how to use it?
It’s hard getting new products and procedures into the market, especially when the market is the whole world. Until we do, we need to start testing, tracking, and quarantining. Everywhere.
Some magic future day, we will need to vaccinate pretty much everyone. Everywhere. Which is a problem because, well, who’s got seven billion needles?
While Bill and Melinda Gates are building redundant vaccine plants to compress the time to market of a successful vaccine, no one’s been paying attention to needles. Vaccine development time compression is for naught unless there are needles to deliver the stuff.
The CEO of medical supply company Becton Dickinson is sounding the needle supply chain alarm.
“Waiting until a vaccine is available will be too late. There is not capacity in the global industry to manufacture hundreds of millions or billions of syringes and needles in a month or two.”
Becton Dickinson spokesman Troy Kirkpatrick, 9 May 2020
Governments can help the private sector with projects like manufacturing billions of needles. Programs to guarantee purchase of large quantities of items needed at once-in-a-lifetime quantities reduce the market risk for manufactures of medical equipment. The US failed to provide effective purchase programs for protective gear and ventilators. It can work with manufacturers to do a better job with needles.
And about the testing, tracking, and quarantining I mentioned above as the next step: How do we do it? Marty’s brother Tom explains. He has some really good ideas.
I’m out of time. I’m ending today on a different bit of technology.
While Covid-19 has been diverting our attention, renewable energy has quietly taken over from coal.
Solar and onshore wind are now the cheapest sources of new-build generation for at least two-thirds of the global population, Bloomberg New Energy Finance said in an April 28 report, while battery storage is now the most cost-effective source of peaking power.
Reuters, “Do renewables hold the upper hand against coal in post-coronavirus world?,” 14 May 2020
With the world economy on its head, energy demand down, and Russia fighting oil prices wars with Saudi Arabia, the energy industry is transforming. New energy production investment will find better returns in renewable solar and wind energy plants than in coal plants.
I write this in part because it’s great news for climate change, but also because of how quickly the transition to renewable energy is happening. There’s a tipping point in energy pricing that has been creeping up for decades as the cost of renewable energy has declined slowly, but relentlessly. The moment the cost of a renewable kWh of electricity drops below the cost of a fossil fuel kWh of electricity is the moment the market switches. In an instant.
I feel that way about the relentless Covid-19 developments. They seem slow in a lockdown, but they are breathtakingly fast. There’s a tipping point in our understanding of the immune system that’s been creeping up for decades. With bioinformatics and DNA sequencing, we’ve reached a stage where the world can respond to a pandemic with over 100 Covid-19 vaccines candidates and over 200 labs developing Covid-19 tests. We are months away from a mAb solution. We have the technology to test, track, and quarantine. We just have to figure out how to get it to everyone that needs it. Everywhere.
Like the renewable energy tipping point, the Covid-19 tipping point is coming soon.